Search This Blog
Please Don't Pass The Nuts™
Just because you have a restricted diet, doesn't mean you have a restricted life.
Posts
Latest Posts

Posted by
Allergic Girl
The Blog May Have Gone Quiet; I Have Not
- Get link
- Other Apps
Posted by
Allergic Girl
Resources for Back to School 2020 & Covid-19
- Get link
- Other Apps

Posted by
Allergic Girl
#FoodAllergyAwarenessWeek 2020 & Organic Valley
- Get link
- Other Apps

Posted by
Allergic Girl
Basic Beef Meatball Recipe: Nut-Free, Gluten-Free, Fish-Free
- Get link
- Other Apps

Posted by
Allergic Girl
Cilantro Lime Chicken Meatball Recipe: Nut-Free, Gluten-Free, Dairy-Free
- Get link
- Other Apps
Posted by
Allergic Girl
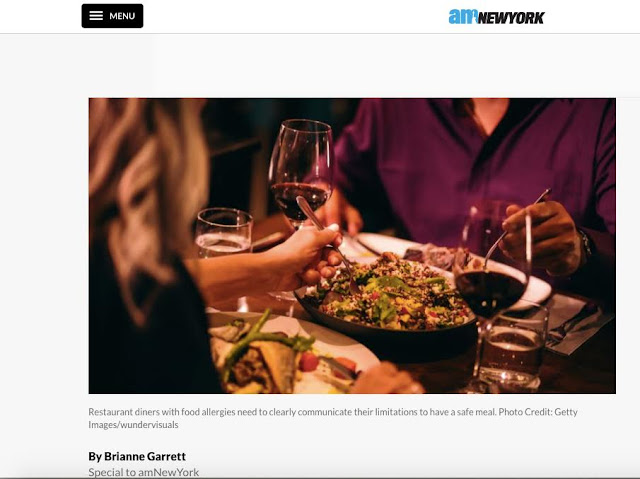
AmNewYork: Tips for eating out in NYC with food allergies with Allergic Girl
- Get link
- Other Apps
Posted by
Allergic Girl
AAAAI: New Research - EpiPen Expiration Dates Too Short
- Get link
- Other Apps

Posted by
Allergic Girl
Recipe: Namaste Foods Scone and Muffin Mix, Nut-Free, Gluten-Free
- Get link
- Other Apps

Posted by
Allergic Girl
Review: Play It Loud: Instruments of Rock & Roll, April 8–October 1, 2019, Met Musuem
- Get link
- Other Apps

Posted by
Allergic Girl
Allergic Girl Event: Food Allergy Connecticut Presents Sloane Miller, Tuesday, April 2, 2019 6:30 PM
- Get link
- Other Apps